History of the Brown Department of Family Medicine
History of the Brown Department of Family Medicine
1811 - 1827 • First Brown Medical School
Brown became the third university in the nation to offer academic medical education. In its brief 16-year history, this program attracted several illustrious teaching physicians. But in 1827, Brown’s president, Francis Wayland, convinced the Corporation to vote that thereafter no member of the faculty should receive his salary unless he occupied a room in the college and helped to preserve order among the rowdy students. As many of the medical professors were generalists living in their communities, they depended on active medical practices for their livelihood and refused the offer. This led to the closure of the school in 1827.

1894 • Memorial Hospital of Rhode Island Founded
The hospital was founded to serve the people of the Blackstone Valley. The funds were from a bequest from William F. Sayles, a businessman and philanthropist who owned mills in Saylesville, Rhode Island. Sayles' son, Frank A. Sayles, decided to build the original 30-bed hospital that started to see patients in the early 1900s. A home for general practitioners, it would later be the site of the first Family Medicine residency in the Ivy League.
1962-1972 • Opening of the Current Brown Medical School
Initially a continuum of four years of undergraduate study and two years of graduate study towards a Master of Medical Science prior to clinical training elsewhere, the program sparked immediate growth in the Brown faculty and staff of collaborating hospitals. By 1972, Brown’s full medical degree program was launched and the first 4-year Medical School class graduated in 1975.

Early 1970s • Planning for the Family Medicine Residency
The CEO of Memorial Hospital of RI, Mr. Frank Dietz, along with a leading faculty member from internal medicine, traveled to one of the early Family Practice residencies in Hunterdon, New Jersey to gather information. Meanwhile, the first Family Medicine Division Head and later second Dean of Brown Medical School, Dr. David Greer, visited the US midwestern heartland to learn about the new specialty in Kansas City and upper Minnesota. The zealous founders of the field, the leaders of the new American Academy of Family Physicians (AAFP), were eager to help Brown make the move to Family Medicine. They imparted their wisdom to Dr. Greer during his visits and later when they came to Pawtucket.
Mid 1970s • Start of the Family Care Center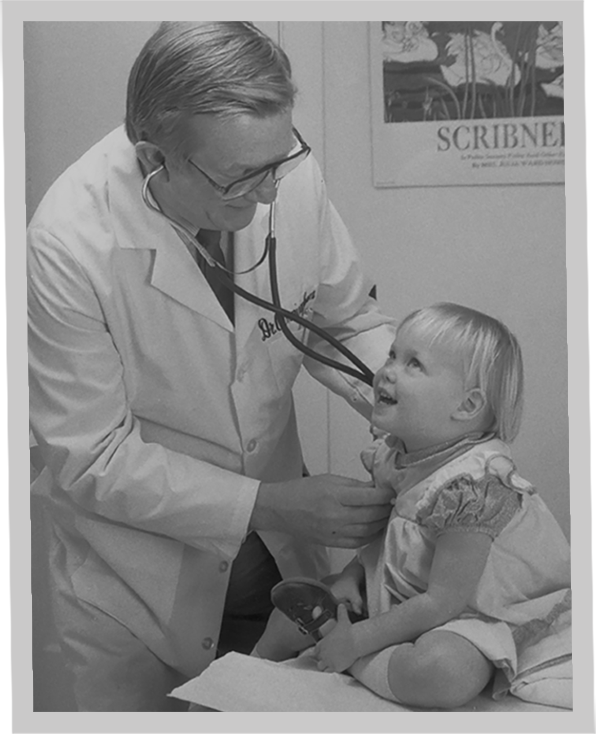
Dr. John J. Cunningham, a leading Pawtucket General Practitioner, moved his general practice (staff, patients, and records) to MHRI and became the first Family Medicine Medical Director.
1975 • Inauguration of the Brown Family Medicine Residency
The newly accredited Family Medicine residency opened on July 1, 1975, with seven trainees. The full-time faculty consisted of Dr. Greer, Dr. Cunningham, Dr. Thomas Scaramella, a psychiatrist who has been the residency director at Butler Hospital, Dr. Mary Ann Passero, a pediatrician, and Dr. John Evrard, an OB-Gyn. A psychologist, Ann DeLancey, joined soon afterward.
1977 • Expansion of the Residency
Family Medicine class size expanded to 12 residents per year.
1978 • Family Medicine Granted Departmental Status by Brown University
This was the first Department of Family Medicine in the Ivy League and was considered a major innovation at Brown.

1978 • First Chair of Family Medicine
Dr. Louis Hochheiser, who had served in the US military and was initially trained in pediatrics, moved into Family Practice early in his career and brought new energy to the Department, which began to expand its range of activities and number of faculty.
1978 • First Family Medicine Residency Graduating Class
Many of the graduates stayed locally, starting a tradition in which most residents go into practice within an hour’s drive of the residency.
1979 • Start of the Family Medicine Predoctoral Division
The goal of this division was to teach Brown medical students the principles of medical care and attract young physicians to the specialty, led by the first Predoctoral Director and later Associate Dean for Education for over twenty years, Dr. Stephen Smith.
 1981 • Launch of the Family Medicine Research Group
1981 • Launch of the Family Medicine Research Group
Though there had previously been scholarship in the Department, the research division started with the arrival of Dr. Larry Culpepper in 1981. He conducted local, national, and international research on topics as varied as otitis media and school- and community-based interventions to improve pregnancy outcomes. This tradition of research in Family Medicine was strengthened when in 1997 the Brown University Center for Primary Care and Prevention was established at MHRI (in a collaboration between Family Medicine, Internal Medicine, and Community Health/Public Health) to improve the health of individuals and communities by promoting research, enriching knowledge, and improving practice in primary care and prevention. Thomas M. Lasater, Ph.D., was its first director and Dr. Chuck Eaton succeeded him and was its first Family Medicine Director starting in 2004.
1986 • Second Chair of Family Medicine
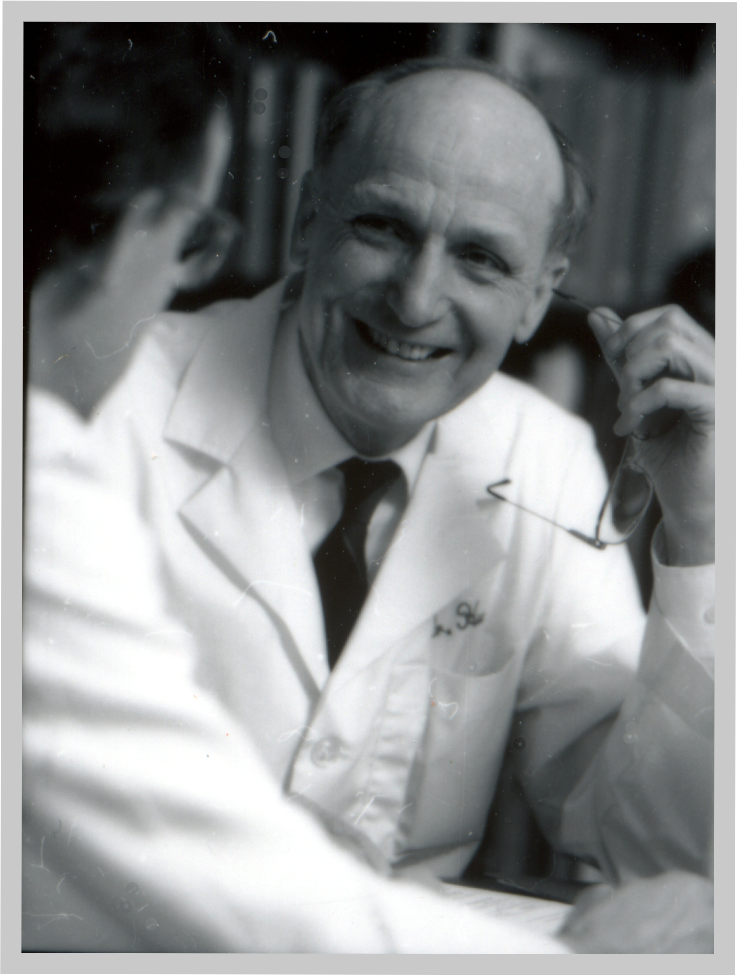
Dr. Vincent Hunt joined the Department as its second Chair in 1986. During his 14-year tenure, he led the Department to new heights, including it being rated the #1 Department in the country.
1991 • Maternal and Child Health (MCH) Fellowship Initiated
The Department’s MCH fellowship was initiated by Dr. Brian Jack and later led by Dr. Rick Long. After a hiatus, it was reborn in 2016 under the leadership of Dr. Sue Magee, training clinical leaders in family-centered Maternal Child Health care. Providing coordinated and comprehensive services to vulnerable and underserved populations.
1992 • Blackstone Valley Community Health Care in Central Falls Becomes an Outpatient Site for the Brown Family Medicine Residency
This important early collaborative arrangement connected the residency to a leading Federally Qualified Health Center (FQHC) serving vulnerable populations. Many of the residents who trained at that site later worked at FQHCs in the state, including serving as their medical directors.
1995 • Family Medicine Becomes a Required Clerkship for all Brown Medical Students
A required six-week clinical rotation in Family Medicine was mandated at Brown under the guidance of Dr. Chuck Eaton.

2001 • Third Chair of Family Medicine
Dr. Jeffrey Borkan served in this position from 2001-2022 and oversaw the expansion and revitalization of the Department and helped meet the challenges to primary care in rough healthcare seas. Dr. Borkan, a Family Physician and medical anthropologist, brought a vision of Family Medicine that included the integration of clinical service, education, research and advocacy.
 2008 • Opening of the Kent Family Medicine Residency
2008 • Opening of the Kent Family Medicine Residency
Family Medicine residency training in RI expanded with the development of the Kent Residency which opened in 2008 and, after moving twice, found a supportive and stable home at Thundermist Health Center in West Warwick. After the founding leadership by Dr. Polly Leonard, it was guided by Dr. Jessica Manyan who as Residency Director from 2008 to 2020 overcame multiple hurdles to create an exciting and effective training program. The residency received Accreditation Council for Graduate Medical Education (ACGME) recognition in 2016.

2010 • Launch of the Brown Global Health Faculty Development Fellowship
The fellowship aims to teach family physicians the additional clinical, teaching, scholarly and leadership skills necessary for work in resource-limited settings.
2013 • Memorial Hospital of RI Acquired by Care New England
After a decade of economic struggles, MHRI sought suitors and, after a long process, was acquired by Care New England (CNE).
2015 • Transformation of the Department to Become More “Statewide”
Faced with both opportunities around the State and the financial deterioration at MHRI, the Department opened adult medicine services at The Miriam Hospital and Kent Hospital, as well as FMOB service at Women & Infants, Kent, and Landmark.

2016-17 • Merger of the Brown and Kent Residencies
The Kent Family Medicine Residency merged with the Brown Family Medicine residency, becoming a second residency site, both under the leadership of Program Director Dr. Fadya El Rayess.
2017-18 • Closure of Memorial Hospital of RI
The Hospital continued to lose ground financially and in terms of inpatient admissions and surgeries and could not be turned around despite the efforts of CNE. The hospital was closed in stages, starting with the beloved Labor and Delivery Department and the last being the Emergency and Rehabilitation Departments. Despite the closure of the hospital, there has been the continuation of outpatient services at the site including the expansion of the Family Care Center.
despite the efforts of CNE. The hospital was closed in stages, starting with the beloved Labor and Delivery Department and the last being the Emergency and Rehabilitation Departments. Despite the closure of the hospital, there has been the continuation of outpatient services at the site including the expansion of the Family Care Center.

2020-23 • COVID-19 Pandemic
Starting in 2020, life changed across the globe as COVID-19 dominated the conversation. The Family Care Center and the Residency responded in multiple ways with faculty, residents, and staff serving as the unsung heroes of the pandemic. Early on the FCC was tasked with running an evaluation unit that was set up in tents in the parking lot to allow safe evaluation of patients. Brown medical students and incoming interns stepped up to do phone triage prior to visits. Through heat waves, chills, and storms, the outdoor unit operated and as testing became available, this service was provided for individuals in cars or who walked up, improving access and care. A ”Team D” with negative pressure rooms was built in part of the old MHRI building, staffed by Family Medicine for patients with suspected COVID. Sometimes up to one-third of the residents and faculty were quarantined during the epidemic, wreaking havoc on clinical services. The response was a joint faculty/resident “Quaranteam” that provided telehealth to patients from across the Blackstone Valley. In addition, family medicine residents and faculty cared for patients with COVID on the inpatient services of Kent, The Miriam, and Women & Infants, as well as at the temporary hospitals set up across the state.

2022 • Fourth Chair of Family Medicine and First Endowed Chair of Family Medicine
Dr. Caroline Richardson was hired in 2022 and received the George A. and Marilyn M. Bray Professor of Family Medicine at Brown University Endowed Chair. She is an internationally recognized researcher and journal editor who was recruited with major support from both CNE and Brown. Working together with our partners, she has been tirelessly striving to improve clinical services, reduce burnout, rationalize the electronic health record, strengthen teaching, and revitalize research in the Department.
2024 • Diabetology Fellowship Begins
The newest fellowship, led by Dr. Leonard Bertheau, is designed to train primary care physicians to be experts in the clinical management of patients with complex diabetes.


